Appendicitis
Appendicitis
Appendicitis is an inflammation of the appendix, a small worm-like pouch attached to the large bowel. It can happen at any age but most cases are between 8 and 25 years of age. For young people, appendicitis is probably the most common cause of stomach pain requiring emergency surgery.
Causes
In most cases, the specific reason for the inflammation is not known but it is due to blocking of the opening connecting the large intestine and appendix. In many cases it is caused by small pieces of hardened stool (faecaliths) that get stuck in the appendix.
Symptoms
The first sign is usually a pain or discomfort in the centre of the abdomen. The pain usually begins near the umbilicus and moves down and to the right. This pain comes and goes in waves and increases on movement. Pain is often thought at first to be a simple stomach upset.
- Nausea
- Vomiting
- Constipation
- Diarrhoea
- Inability to pass gas
- Low fever that begins after other symptoms
- Abdominal swelling
- Anorexia
Diagnoses
- The doctor takes a medical history from the patient and checks their temperature
- Blood and urine tests are performed to look for infection
- The doctor examines the patient by pressing on the lower right part of the abdomen and sometimes by inserting a finger in the anus (back passage) in order to exclude other causes of pain
- Women are often given a vaginal examination
There is no one test that will diagnose appendicitis with certainty, usually doctors use CT scan or ultrasound to see whether the appendix looks inflamed. Surgery is performed on the basis of the doctor’s examination and results of the tests. Many diseases can cause the same symptoms as appendicitis.
Course of illness
The inflammation can cause infection, a blood clot, or rupture of the appendix. Because of the risk of rupture, appendicitis is considered an emergency. Anyone with symptoms needs to see a doctor immediately.
Treatment
- Surgical removal of the appendix (appendicectomy) is the most common procedure. A 3-6cm horizontal incision is made in the lower part of the abdomen on the right side, through which the appendix is removed
- In some hospitals, the appendix is routinely removed by a keyhole operation or the insertion of a three-fibre optic camera through the stomach (laparoscopy)
In uncomplicated cases, a two to three day hospital stay is typical. The person can go home when their temperature is normal and their bowel starts to function again. The stitches are removed 10 days after the operation. A return to ordinary daily life within four to six weeks is usual.
Cancer
What is Cancer?
Cancer is a disease that results from abnormal growth and division of cells that make up the body’s tissues and organs. Under normal circumstances, cells reproduce in an orderly fashion to replace old cells, maintain tissue health and repair injuries.
However, when growth control is lost and cells divide too much and too fast, a cellular mass -or “tumor” -is formed.
If the tumor is confined to a few cell layers and it does not invade surrounding tissues or organs, it is considered benign. By contrast, if the tumor spreads to surrounding tissues or organs, it is considered malignant, or cancerous. In order to grow further, cancer develops its own blood vessels and this process is called angiogenesis. When it first develops, a malignant tumor may be confined to its original site.
If cancerous cells are not treated they may break away from the original tumor, travel, and grow within other body parts, the process is known as metastasis.
Cancer Screening is the performance of tests on apparently well people in order to detect a medical condition at an earlier stage.
Click on the below links to find more about the individual cancers.
- Esophageal cancer
- Liver cancer
- Pancreatic cancer
- Colorectal cancer
- Breast cancer
- Gastric cancer
Cholecystectomy
Of all surgical procedures for which laparoscopy is an option, cholecystectomy – gallbladder removal – is the most widely recognized.
Cholecystectomy is the surgical removal of the gallbladder. Using advanced laparoscopic technology, it is now possible to remove the gallbladder through a tiny incision in front of the abdomen.
A specialist trained in laparoscopic procedures will recognize any adjunct problems encountered, and be in a position to deal with them, for example, adhesions, cysts, or hernias.
Indications for Laparoscopic Gall Bladder removal (Cholecystectomy)
- If an attack hasn’t settled after 12 hours
- If there are complications such as jaundice, pancreatitis
- If patient suffers recurrent pain or vomiting
- If patient suffers cholangitis
What are the Benefits?
The main benefit of this procedure is that it is minimally invasive surgery. Minimally invasive surgery means “Less Pain” and “Faster Recovery”.
There is no incision pain as occurs with standard abdominal surgery. So the recovery time is much quicker. Also, there is no scar on the abdomen.
Is laparoscopy always advised?
There are very few instances when laparoscopic surgery is not preferable to conventional surgery for cholecystectomy. This is especially true when the surgical and nursing team is well experienced in the procedures and post-operative care.
The only real contraindication is if the anesthetic risk is too high. Other, lesser contraindications – such as during the first trimester of pregnancy – need not pose a problem to the experienced laparoscopic surgeon.
Risks & Complications
Like any abdominal surgery, Laparoscopic Cholecystectomy carries some risks. Even though infrequent, it still carries some of the same risks as general surgery. Current medical reports indicate that the low complication rate is about the same for this procedure as for standard gallbladder surgery.
Complications are rare and may include:
- Bleeding & infection may occur but is rare with experienced surgeons
- In a few cases, the gallbladder cannot be safely removed by laparoscopy. Standard open abdominal surgery is then immediately performed
- Nausea and vomiting may occur after the surgery
- Injury to the bile ducts, blood vessels, or intestine can occur, requiring corrective surgery
Esophagitis
Alternative names: Indigestion and Heartburn
The term ‘indigestion’ is a layman’s term and is used to cover the symptoms of a few different medical conditions.
Medical conditions that are often described as ‘indigestion’ and which have ‘indigestion’ as a symptom are:
- Heartburn (gastro-oesophageal reflux)
- Ulcers
- Non-ulcer dyspepsia (when you have symptoms of an ulcer but no sign of ulcer on investigation)
- Food intolerance, e.g. lactose intolerance
- Bloating and flatulence and
- Aerophagia (swallowing excessive amounts of air)
Many people with indigestion suffer in silence, sometimes for years, receiving little or no medical treatment apart from over-the-counter antacids.
While these are very effective in medicating heartburn, there are now many more medications available, which can provide perfect symptomatic relief.
There is also a greater awareness that acid reflux which causes the heartburn may damage the lining of the esophagus and increase the potential for serious health problems due to the process of chronic inflammation.
It is becoming increasingly important to treat your symptom of heartburn less casually and discuss the prospects for treatment with your doctor.
Hemorrhoids
Hemorrhoids are one of the most common ailments known in both men and women, but many suffer in silence rather than discuss hemorrhoid treatment with their doctor.
The American Society of Colon and Rectal Surgeons reports that 50 percent of all Americans will have hemorrhoids in their lifetime. One reason people do not talk about hemorrhoid problems with their doctor is because they anticipate a painful, traditional hemorrhoid surgery.
Click here for more information about Hemorrhoids from the National Digestive Diseases Information Clearinghouse.
Hernias
A hernia is a weakness or defect in the abdominal wall. It may be present from birth or develop over a period of time. If the defect is large enough, abdominal contents such as the bowels may protrude through the defect causing a lump or bulge felt by the patient.
Hernias develop at certain sites which have a natural tendency to be weak; the groin, umbilicus (belly button), and previous surgical incisions.
Signs and Symptoms
- Lump in groin area when standing/straining & disappears when reclining
- Pain at the site of the lump, especially when lifting a heavy object
- Swelling of the scrotum
- Excruciating abdominal pain (if you have strangulation)
- Nausea, vomiting, loss of appetite & pain (if intestinal obstruction occurs)
Course of Hernia
Once a hernia has developed, it will tend to enlarge and cause discomfort. If a loop of bowel gets caught in the hernia, it may become obstructed or its blood supply may be cut off. This could then become a life-threatening situation. Since hernias can be repaired effectively and with minimal risk, most surgeons, therefore, recommend that hernias be repaired when diagnosed, unless there is a serious medical problem which makes it too risky.
Treatment
Hernia repair (Surgery)
The standard method of hernia repair involves making an incision in the abdominal wall. Normal healthy tissues are cut until the area of weakness is found. This area, the hernia, is then repaired with sutures. Often a prosthetic material, such as mesh, or another plastic material, is sutured in place to strengthen the area of weakness. Finally, the skin and other healthy tissues that were cut at the beginning are sutured back together to complete the repair.
Newer hernia repair involves minimally invasive laparoscopic techniques. However, hernia operation with open techniques is still a valid option reaching the highest standards of care. Laparoscopic techniques for hernia repair are especially attractive when patients are dealing with recurrent hernias or bilateral inguinal hernias.
Gallstones
A gallstone is a lump of hard material usually ranging in size from a grain of sand to 3-4 cms. They are formed inside the gallbladder as a result of precipitation of cholesterol and bile salts from the bile.
Types of gallstones and causes
- Cholesterol stones
- Pigment stones
- Mixed stones – the most common type. They are comprised of cholesterol and salts
Cholesterol stones are usually yellow-green and are made primarily of hardened cholesterol. They account for about 80 percent of gallstones. Scientists believe cholesterol stones form when bile contains too much cholesterol, too much bilirubin, or not enough bile salts, or when the gallbladder does not empty as it should for some other reason.
Pigment stones are small, dark stones made of bilirubin. The exact cause is not known. They tend to develop in people who have cirrhosis, biliary tract infections, and hereditary blood disorders such as sickle cell anemia in which too much bilirubin is formed.
Other causes are related to excess excretion of cholesterol by liver through bile. They include the following:
- Gender. Women between 20 and 60 years of age are twice as likely to develop gallstones as men.
- Obesity. Obesity is a major risk factor for gallstones, especially in women.
- Estrogen. Excess estrogen from pregnancy, hormone replacement therapy, or birth control pills Cholesterol-lowering drugs.
- Diabetes. People with diabetes generally have high levels of fatty acids called triglycerides.
- Rapid weight loss. As the body metabolizes fat during rapid weight loss, it causes the liver to secrete extra cholesterol into bile, which can cause gallstones.
Symptoms
Many people with gallstones have no symptoms. These patients are said to be asymptomatic, and these stones are called “silent stones.” Gallstone symptoms are similar to those of heart attack, appendicitis, ulcers, irritable bowel syndrome, hiatal hernia, pancreatitis, and hepatitis. So accurate diagnosis is important.
Symptoms may vary and often follow fatty meals, and they may occur during the night.
- Abdominal bloating
- Recurring intolerance of fatty foods
- Steady pain in the upper abdomen that increases rapidly and lasts from 30 minutes to several hours
- Pain in the back between the shoulder blades
- Pain under the right shoulder
- Nausea or vomiting
- Indigestion & belching
Diagnoses
Ultrasound is the most sensitive and specific test for gallstones.
Other diagnostic tests may include
- Computed tomography (CT) scan may show the gallstones or complications
- Endoscopic retrograde cholangiopancreatography (ERCP). The patient swallows an endoscope–a long, flexible, lighted tube connected to a computer and TV monitor. The doctor guides the endoscope through the stomach and into the small intestine. The doctor then injects a special dye that temporarily stains the ducts in the biliary system. ERCP is used to locate and remove stones in the ducts
- Blood tests. Blood tests may be used to look for signs of infection, obstruction, pancreatitis, or jaundice
- In the event of negative ultrasound, a CCK HIDA Scan may be ordered to screen for a non-functioning gallbladder
Course of illness
Bile-duct blockage and infection caused by stones in the biliary tract can be a life-threatening illness. With prompt diagnosis and treatment, the outcome is usually very good.
Complications
The obstruction caused by gallstone may lead to Biliary colic, Inflammation of gallbladder (Cholecystitis). Other complications may include
- Cirrhosis- Cirrhosis is the result of chronic liver disease that causes scarring of the liver (fibrosis – nodular regeneration) and liver dysfunction
- Cholangitis- Cholangitis is an infection of the common bile duct, which carries bile (which helps in digestion) from the liver to the gallbladder and then to the intestines
Treatment
Surgery
Surgery to remove the gallbladder is the most common way to treat symptomatic gallstones. The most common operation is called laparoscopic cholecystectomy. For this operation, the surgeon makes several tiny incisions in the abdomen and inserts surgical instruments and a miniature video camera into the abdomen. The camera sends a magnified image from inside the body to a video monitor, giving the surgeon a close-up view of the organs and tissues. While watching the monitor, the surgeon uses the instruments to carefully separate the gallbladder from the liver, ducts, and other structures.
If gallstones are in the bile ducts, the physician (usually a gastroenterologist) may use endoscopic retrograde cholangiopancreatography (ERCP) to locate and remove them before or during the gallbladder surgery.
Peritonitis
Peritonitis is an inflammation of the peritoneum, which is the membrane that lines the wall of the abdomen and covers the abdominal organs.
Causes, incidence, and risk factors
Types of peritonitis include:
- Spontaneous Peritonitis – an infection that occurs as a complication of ascites (a collection of fluid in the peritoneal cavity), which is usually related to liver or kidney failure
- Secondary Peritonitis – caused by another condition, most commonly the spread of an infection from the digestive organs or bowels
- Dialysis-associated Peritonitis – This is an acute or chronic inflammation (irritation and swelling) of the peritoneum (lining of the abdominal cavity) that occurs in people receiving peritoneal dialysis
Intra-abdominal abscess (abdominal abscess). This condition involves a collection of pus in the abdomen and may cause peritonitis. Before peritonitis develops, it can still cause symptoms that are similar or identical to peritonitis.
- An intra-abdominal abscess may arise following:
- Localization of peritonitis
- Gastrointestinal perforation
- Anastomotic Leak
- Hematogenous (bloodstream) spread
- Sites of gravitational drainage
- Pelvis
- Subhepatic spaces
- Subphrenic spaces
- Paracolic gutters
Symptoms
- Nausea
- Vomiting
- Abdominal pain, which increases on movement
- Abdominal tenderness
- Abdominal distension
- Fever
- Low urine output
- Point tenderness
- Thirst
- Fluid in the abdomen
- Constipation
- Inability to pass feces gas
- Signs of shock in extreme cases
Diagnoses
- Physical examination and medical history
- Blood tests including blood culture and X-rays or CT scans may be ordered
- Peritoneal fluid analysis( paracentesis) & culture
Treatment
The cause must be identified and treated promptly.
Treatment typically involves fluid infusion to control shock, surgery to drain the peritoneal cavity and repair the cause, and antibiotics to deal with the infection. In cases associated with peritoneal dialysis, antibiotics may be infused through the dialysis catheter, but if the infection is severe, the catheter itself must often be removed.
Treatment typically involves surgery and antibiotics.
Course of illness
The outcome is often good with treatment but can be poor without treatment.
Sometimes the outcome is poor even with prompt and adequate treatment.
Complications
Peritonitis can be life-threatening and cause a number of different complications, depending on the type.
Complications may include
- Peritonitis stops the movement of bowel contents (peristalsis), which can block the bowel (paralytic ileus)
- Septic shock – Fluid from the blood accumulates in the abdominal cavity and the loss of fluid from the circulation may also cause shock
- Abscess
- Intraperitoneal adhesions
What Should You Do?
Go to the Hospital emergency room or call 911 if you have symptoms that may indicate peritonitis, as this is a medical emergency.
Pancreatitis
Pancreatitis is an inflammation of the pancreas. The pancreas is a large gland behind the stomach and closes to the duodenum. The duodenum is the upper part of the small intestine. The pancreas secretes digestive enzymes into the small intestine through a tube called the pancreatic duct. These enzymes help digest fats, proteins, and carbohydrates in food. The pancreas also releases the hormones insulin and glucagon into the bloodstream. These hormones help the body use the glucose it takes from food for energy.
Normally, digestive enzymes do not become active until they reach the small intestine, where they begin digesting food. But if these enzymes become active inside the pancreas, they start digesting the pancreas itself. This process is called autodigestion and causes swelling, hemorrhage, and damage to the blood vessels. An attack may last for 2 days.
Types
- Acute pancreatitis occurs suddenly and lasts for a short period of time and usually resolves. Acute pancreatitis is usually caused by drinking too much alcohol or by gallstones. A gallstone can block the pancreatic duct, trapping digestive enzymes in the pancreas and causing pancreatitis.
- Chronic pancreatitis does not resolve itself and results in a slow destruction of the pancreas. Chronic pancreatitis occurs when digestive enzymes attack and destroy the pancreas and nearby tissues. Chronic pancreatitis is usually caused by many years of alcohol abuse, excess iron in the blood, and other unknown factors. However, it may also be triggered by only one acute attack, especially if the pancreatic ducts are damaged.
Either form can cause serious complications. In severe cases, bleeding, tissue damage, and infection may occur. Pseudocysts, accumulations of fluid and tissue debris, may also develop. And enzymes and toxins may enter the bloodstream, injuring the heart, lungs, and kidneys, or other organs.
Acute pancreatitis generally causes severe pain and the sufferer will need emergency treatment in a hospital. Pancreatitis is generally diagnosed quickly, by examination of the abdomen, and confirmed using a series of medical tests, including:
- General tests – such as blood tests, physical examination, and x-rays
- Ultrasound – sound waves form a picture that detects the presence of gallstones
- CT scan – a specialized x-ray takes three-dimensional pictures of the pancreas
Complications
Some of the complications from pancreatitis are low blood pressure, heart failure, kidney failure, ARDS (adult respiratory distress syndrome), diabetes, ascites (accumulation of fluid in the abdomen) and cysts or abscesses in the pancreas.
Treatment options
Treatment depends on the causes and severity of the condition, but may include:
Acute pancreatitis
- Hospital care – in all cases of acute pancreatitis
- Intensive care in hospital – in cases of severe acute pancreatitis
- Fasting and intravenous fluids – until the inflammation settles down
- Esophagus – a thin tube is inserted through your esophagus to allow the doctor to see your pancreas
- Surgery – if gallstones are present, removing the gallbladder will help prevent further attacks. In rare cases, surgery is needed to remove damaged or dead areas of the pancreas
- Lifestyle change – eliminating alcohol
Chronic pancreatitis
- Lowering fat intake
- Supplementing digestion by taking pancreatic enzyme tablets with food
- Eliminating alcohol
- Insulin injections, if the endocrine function of the pancreas is compromised
- Analgesics for pain
Reflux
Gastro Esophageal Reflux Disease (GERD)
The esophagus carries food from the mouth to the stomach. The lower esophageal sphincter is a ring of muscle at the bottom of the esophagus that acts like a valve between the esophagus and stomach.
Gastro Esophageal reflux disease, or GERD, is a chronic disease that occurs when the lower esophageal sphincter does not close properly and stomach contents leak back, or reflux, into the esophagus.
When refluxed stomach acid touches the lining of the esophagus, it causes a burning sensation in the chest or throat called heartburn. The fluid may even be tasted in the back of the mouth, and this is called acid indigestion. Occasional heartburn is common but does not necessarily mean one has GERD. Heartburn that occurs more than twice a week may be considered GERD, and it can eventually lead to more serious health problems.
Anyone, including infants, children, and pregnant women, can have GERD.
Symptoms
The main symptoms are persistent heartburn and acid regurgitation. Some people have GERD without heartburn. Instead, they experience pain in the chest, hoarseness in the morning, or trouble swallowing. You may feel like you have food stuck in your throat or like you are choking or your throat is tight. GERD can also cause a dry cough and bad breath.
The most frequent symptoms of GERD are so common that they may not be associated with a disease. Self-diagnosis can lead to mistreatment. Consultation with a physician is essential to proper diagnosis and treatment of GERD.
Causes
- Hiatal hernia- hiatal hernia occurs when the upper part of the stomach is above the diaphragm, the muscle wall that separates the stomach from the chest
- Alcohol use
- Overweight
- Pregnancy
- Smoking
Also, certain food and drinks are associated with reflux
Diagnoses
- Medical history
- Response to Omeprazole
- A recent study demonstrated a potential role for a proton pump inhibitor, omeprazole, in the diagnosis of GERD
- Barium swallow radiograph
- Uses x rays to help spot abnormalities such as a hiatal hernia and severe inflammation of the esophagus
- Endoscopy
Treatment
Conservative treatment
- Lifestyle modification
- Medications including antacids, Foaming agents, H2 receptor blockers, Proton Pump Inhibitors
Surgical treatment
Surgery is an option when medicine and lifestyle changes do not work. Surgery may also be a reasonable alternative to a lifetime of drugs and discomfort.
Laparoscopic Nissen Fundoplication
This surgery is performed under general anesthesia.
If a combination of lifestyle changes and drug therapy does not remedy reflux symptoms, a Nissen Fundoplication can be a very effective surgical procedure to correct reflux. This procedure involves wrapping the upper portion of the stomach around the base of the esophagus to reinforce the strength of the lower esophageal sphincter. Until recently, the procedure required a large abdominal incision. A hospital stay of 3-5 days was usually required, and the time to full recovery and return to work was measured in weeks.
A laparoscopic Nissen Fundoplication is a minimally invasive approach that involves specialized video equipment and instruments that allow a surgeon to perform the procedure through four tiny incisions, most of which are less than a half-centimeter in size. One advantage of this method is a brief hospitalization. Most of the time it will require an overnight stay. Other advantages include less pain (less of a need for pain medication), fewer and smaller scars, and a shorter recovery time.
Laparoscopic Nissen Fundoplication is a safe and effective treatment of GERD. However, in rare cases, the laparoscopic approach is not possible because it becomes difficult to visualize or handle organs effectively. In such instances, the traditional incision may need to be made to safely complete the operation.
Breast Conditions
Abnormal Nipple Discharge
Alternative names
Discharge from breasts; Milk secretions; Lactation – abnormal; Witches milk; Galactorrhea
Definition
This symptom involves abnormal discharge from the nipple(s)
Considerations
The likelihood of nipple discharge increases with age and number of pregnancies.
While a milky nipple discharge is rare in men and in women who have never been pregnant, it does occur. When it does, it is likely to be caused by some underlying disease, particularly when accompanied by other changes in the breast(s).
It is relatively common in women who have had at least one pregnancy. A thin yellowish or milky discharge (colostrum) is normal in the final weeks of pregnancy.
The nature of the discharge can range in colour, consistency, composition, and may occur on one side or both sides.
“Witch’s milk” is a term used to describe nipple discharge in a newborn. The discharge is a temporary response to the increased levels of maternal hormones. Witch’s milk should disappear within 2 weeks as hormone levels dissipate in the newborn.
Other nipple discharges can be bloody or purulent (containing pus), depending on the cause.
Common Causes
- Breast abscess (most common in lactating women)
- Trauma can cause discharge from both breasts
- Drugs such as cimetidine, methyldopa, metoclopramide, oral contraceptives, phenothiazines, reserpine, tricyclic antidepressants, or verapamil
- Prolactinoma (prolactin-secreting tumour in the brain)
- Intraductal papilloma (a small noncancerous growth in the duct of the breast)
- Ductal ectasia
Home Care
Follow provider-prescribed therapy.
Call your health care provider if
If there is any abnormal nipple discharge, call your healthcare provider.
What to expect at your health care provider’s office
The medical history will be obtained and a physical examination performed.
Medical history questions documenting a nipple discharge in detail may include:
- Are you pregnant?
- Are you breastfeeding?
- What type of drainage is there?
- Does it look like milk (even though you are not breastfeeding)?
- Does it look bloody?
- Does it look like pus?
- Is the drainage from both breasts?
- How much drainage is there?
- Enough to stain the lining of the bra?
- Enough to soak through the bra?
- Does the discharge occur spontaneously, or only when expressed?
- Do you perform breast self-examination? How often?
- What medications do you take?
- What other symptoms are also present? Especially is there:
- Fever
- A breast lump
- Breast pain
- Headaches or change in vision
The physical examination will include an examination of the breasts for lumps or other abnormality.
Diagnostic tests that may be performed include:
- Breast biopsy (if lump is found)
- Cytologic study of discharge (a study of the cells in the discharge)
- Head CT scan to look for pituitary tumour
- Mammography
- Serum prolactin
- Transillumination (a light is placed against the breast to help determine if there is an accumulation of fluid in the tissue)
- Ultrasonography (ultrasound of the breast)
Breast Anatomy
Attitudes about women’s breasts have always been influenced by fashion trends. In the Twenties, women bound their breasts; in the Forties, more volume was desirable; then, in the Sixties, a less restricted look was popular. Contemporary styles reflect a trend toward fuller, yet natural-looking lines. But regardless of your breast size, all healthy breasts have the same basic anatomy. When you’re considering breast reduction, it helps to know your anatomy so you can make informed choices with your surgeon’s guidance.
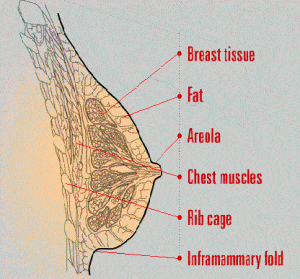
Breast tissue is made up of glands that produce milk during pregnancy.
Fat provides protective padding for the milk-producing glands.
The areola is the pigmented tissue that surrounds each nipple.
Chest muscles contract and expand so you can move your arms.
The rib cage houses vital organs like your heart and lungs.
The Inframammary fold is the crease where your chest wall meets your breast.
Breast Biopsy
Once a breast lump or breast abnormality has been detected, your doctor may want to conduct a breast biopsy. This procedure involves taking sample tissue from the suspicious area to determine whether the breast lump is cancerous.
While the thought of having a breast biopsy might be frightening, the results can provide reassuring peace of mind. Remember, the vast majority of breast biopsies do not turn out to be breast cancer. And a biopsy is currently the only way to achieve an accurate breast cancer diagnosis.
There are various breast biopsy options to consider. The choices range from an open surgical procedure to new minimally invasive techniques. Be sure to understand your biopsy options and talk with your doctor to determine the procedure that is best for you.
There are two methods for producing images in minimally invasive breast biopsies:
- Stereotactic
- Ultrasound guided
Stereotactic biopsy
Stereotactic [STARE-ee-o-TAK-tik] biopsies use mammography (x-rays) to locate breast abnormalities, while ultrasound biopsies use high-frequency sound waves to create breast tissue images.
In a minimally invasive breast biopsy using stereotactic imaging, a patient lies face down on a special table with her breast protruding through a hole in the table’s surface. The breast is lightly compressed to immobilize it throughout the biopsy procedure. The table is connected to a computer that produces detailed x-ray images of the abnormality to be biopsied. Using these images, the doctor guides a special sampling device (for example, biopsy probe) to collect tissue specimens.
Ultrasound-guided biopsy
Minimally invasive breast biopsies using ultrasound imaging are performed on patients in an upright or reclined position. Using a hand-held transducer, a doctor will move the device back and forth across the breast to generate clear images of the abnormal breast tissue.
While viewing the images on a computer monitor, the doctor will guide a small probe into the breast to retrieve sample tissue specimens.
Core Needle Breast Biopsy
In a core needle biopsy, the physician makes a small skin incision through which a needle is inserted into the lesion to obtain sample tissue. The hollow spring-loaded device is “fired” repeatedly into the abnormality to collect a sufficient amount of breast tissue for analysis. Usually, 4 to 6 samples are taken (4 to 6 insertions). This biopsy procedure is performed in an outpatient setting or doctor’s office without general anesthesia or stitches.
Fine Needle Aspiration Breast Biopsy
Fine Needle Aspiration (FNA) is a biopsy procedure that uses a thin needle on a syringe to draw fluid and/or cellular material from a breast abnormality. Thus, Fine Needle Aspiration provides information about cellular material, whereas the other tissue biopsy procedures allow tissue within the abnormality to be compared to surrounding tissue for a more accurate diagnosis. Fine Needle Aspiration is most often used to aspirate, or drain fluid, from benign (non-cancerous) fluid-filled cysts. However, the extracted fluid can be examined by a pathologist to confirm whether the abnormality is benign or requires further testing.
Fine Needle Aspiration biopsy procedures are generally performed by a physician in his or her office. If the breast lump is small and cannot be felt, the procedure can be performed using stereotactic or ultrasound imaging guidance. During the procedure, a long, thin needle is inserted through the breast into the abnormality for sample extraction. Because the needles used for Fine Needle Aspiration biopsies are smaller than needles used to draw blood, local anesthesia is not required.
Breast Cancer
Why should I be concerned about breast cancer?
It seems like we’ve all been affected by breast cancer at some point in our lives, whether we have had it, or have had a family member or friend who’s battled it. Every woman has a chance of getting breast cancer. Other than skin cancer, breast cancer is the most common cancer in American women and the disease we fear most. As scared as we are, you can try to remember that if you find breast cancer early, it can often be treated successfully. Many women have overcome breast cancer and are living life to its fullest!
Where can I learn more about breast cancer?
For More Information…
National Cancer Institute
Cancer Information Service
Tel: (800) 422-6237
Website: www.cancer.gov
National Breast and Cervical Cancer Early Detection Program
Tel: (888) 842-6355 (select option 7)
Website: www.cdc.gov
American Cancer Society
Tel: (800) ACS-2345
Website: www.cancer.org
Susan G. Komen Breast Cancer Foundation
Tel: (800) 462-9273
Website: www.komen.org
Breast Cancer Screening
The goal of screening exams for early breast cancer detection is to find cancers before they start to cause symptoms. Screening refers to tests and examinations used to detect a disease, such as cancer, in people who do not have any symptoms. Early detection means applying a strategy that results in an earlier diagnosis of breast cancer than otherwise might have occurred.
Breast cancers that are detected (found) because they are causing symptoms tend to be relatively larger and are more likely to have spread beyond the breast. In contrast, breast cancers found during screening exams are more likely to be small and still confined to the breast.
The size of a breast cancer and how far it has spread are the most important factors in predicting the prognosis (the outlook for chances of survival) of a woman with this disease. Finding a breast cancer as early as possible greatly improves the likelihood that treatment will be successful. There is no question that early detection tests for breast cancer save many thousands of lives each year, and that many more lives could be saved if even more women and their health care providers took advantage of these tests.
Breast Cancer screening includes a Breast Self Examination, Breast X-ray (mammogram) and professional physical examination.
Breast Infection- Mastitis
Alternative names
Mastitis; Infection – breast tissue; Breast abscess
Definition
This infection is located in the tissue of the breast. In most cases, bacteria entered the tissue through cracks in the nipples.
Causes, incidence, and risk factors
Breast infections are usually caused by a common bacteria found on normal skin (Staphylococcus aureus). The bacteria enter through a break or crack in the skin, usually the nipple.
The infection then takes place in the parenchymal (fatty) tissue and causes swelling of the parenchymal tissue outside the milk ducts. This swelling compresses on the milk ducts, and the result is pain and swelling of the infected breast.
Breast infections usually occur in women who are breastfeeding. Breast infections that are not related to breastfeeding must be differentiated from a rare form of breast cancer.
Symptoms
- breast pain
- breast lump
- breast enlargement on one side only
- swelling, tenderness, redness, and heat in breast tissue
- nipple discharge (may contain pus)
- nipple sensation changes
- itching
- tender and/or enlarged lymph nodes in armpit on the same side
- fever
Signs and tests
In women who are not breastfeeding, testing may include mammography or breast biopsy. Otherwise, tests are usually not necessary.
Treatment
Self-care may include applying moist heat to the infected breast tissue for 15 to 20 minutes four times a day.
Antibiotic medications are usually very effective in treating mastitis. You are encouraged to continue to breastfeed or to pump to alleviate engorgement while receiving treatment.
Support Groups
The stress of an illness can often be helped by joining a support group in which members share common experiences and problems. See breastfeeding – support group.
Expectations (prognosis)
The condition usually clears quickly with antibiotic therapy.
Complications
In severe infections, an abscess may develop. Abscesses require more extensive treatment, including incision and drainage. Discontinuation of breast-feeding may be recommended in this case.
Calling your health care provider
Call your health care provider if any portion of the breast tissue becomes reddened, tender, swollen, or hot, or if the lymph nodes in the armpit become tender and/or enlarged.
Prevention
Good breast care, especially after delivery and while breast-feeding, may decrease the potential to develop breast infections.
Breast Pain
Alternative names
Pain – breast; Mastalgia; Mastodynia; Breast tenderness
Definition
Breast pain involves any discomfort or pain in the breast, such as premenstrual tenderness.
Considerations
There are many possible causes for breast pain. For example, hormonal fluctuations related to menstruation or pregnancy are often responsible for breast tenderness. Some degree of swelling and tenderness just before your period is normal. The question is how tolerable (or intolerable) the discomfort is to you.
Although many women with pain in one or both breasts understandably fear breast cancer, breast pain is NOT a common symptom of cancer.
Boys and men have breast tissue. If a male has breast tissue that is visible, this is called gynecomastia. As a normal part of development, adolescent boys can have some breast swelling and tenderness. Like breast tenderness in women, this is due to hormonal changes.
Common Causes
Some degree of breast tenderness is normal, caused by hormonal fluctuations from:
- Menstruation
- Pregnancy — tends to be more common during the first trimester and pregnancy at a young age
- Puberty — in both girls and boys
- Breastfeeding
- Approach of menopause (once your menstrual periods have stopped completely, breast tenderness often goes away unless you are taking hormone replacement therapy)
Soon after childbirth, your breasts may become engorged with milk. This can be very painful and is usually accompanied by swelling. If you also have an area of redness, call your healthcare provider.
Other common causes of breast pain include:
- Fibrocystic breast changes
- Mastitis — a blocked and infected milk duct that may have some redness, usually associated with breastfeeding
- Premenstrual syndrome (PMS)
- Alcoholism with liver damage
- Injury
Fibrocystic breast tissue is a common condition. It involves breast lumps and bumps throughout the breast tissue that tend to be more tender just before your menstrual period.
Certain medications may also cause breast pain, including digitalis preparations, aldomet, aldactone and other potassium-sparing diuretics, anadrol, and chlorpromazine.
Shingles can lead to pain felt in the breast if the painful blistering rash appears on the skin over one of your breasts.
Home Care
For tips on how to manage pain from fibrocystic breasts, see breast lumps.
Talk to your doctor about possibly taking birth control pills. These can help relieve pain.
If you have a breast infection, you will need antibiotics. Look for signs of infection like localized redness, nipple discharge, or fever. Contact your doctor if you have these signs.
Just after an injury to the breast occurs, apply a cold compress such as an ice pack (wrapped in a cloth — don’t apply directly to the skin) for 15 to 20 minutes. Take a nonsteroidal anti-inflammatory drug (NSAID) such as ibuprofen to reduce the likelihood of developing persistent breast pain or swelling.
Call your doctor if you have:
- Discharge from your nipples, especially blood or pus
- Given birth within the last week and your breasts are swollen or hard
- Signs of a breast infection, including localized redness, pus, or fever
- Noticed a new lump associated with the pain that does not go away after your menstrual period
- Persistent, unexplained breast pain
What to expect at your health care provider’s office
Your health care provider will perform a breast examination and ask questions about your breast pain, such as:
- How long have you had the symptoms?
- Are one or both of your breasts affected?
- Do you have any nipple discharge?
- Do you perform breast self-examination?
- Have you noticed any lumps or anything unusual when you examine your breasts?
- When was your last mammogram?
- What other symptoms are present? Do you have a fever?
- What medication are you currently taking?
Diagnostic tests that may be performed include the following:
- Breast biopsy
- Culture of nipple discharge to test for infection
- Cytology (microscopic evaluation) of nipple discharge
- Mammography
- Fine needle aspiration — a small needle is inserted into the breast to remove fluid that may have collected in a cyst (usually not cancerous)
Treatment may include the following:
- Pain relievers may be prescribed
- Changes to your diet may be suggested
- Certain medications may be changed or discontinued
Your health care provider should schedule a follow-up visit in case the symptoms have not resolved in a given period of time. He or she may recommend consultation with a specialist if the symptoms do not go away or if you have a complicated condition.
Prevention
Wear a well-fitting brassiere for support, especially if your breasts are large.
Perform a monthly breast self-exam 3-5 days after your period (when the breast tissue is the least tender). This is important to feel for any changes in your breast tissue. If you detect any change from the previous month, it is important to notify your doctor.
Breast Self Examination BSE
Why should I do a breast self-exam?
Regular breast self-exam can help you know how your breasts normally feel and look, so you can notice any changes. When you find a change, you should see your healthcare provider. Most breast changes or lumps are not cancerous, but only a health care provider can tell you for sure. When breast cancer is found early, you have more treatment choices and a better chance of recovery. So, it is important to find breast cancer as early as possible.
Breast self-exam should not take the place of getting regular mammograms. Right now, mammograms are the best way to find breast cancer early and to improve your chances for survival.
What am I looking for when I do a breast self-exam?
You are looking for a lump or change that stands out as different from the rest of your breast tissue. If you find a lump or other change in your breast, either during breast self-exam or by chance, you should examine the other breast. If both breasts feel the same, the lumpiness is probably normal. As you get to know your breasts better by doing breast self-exams, you should be able to tell the difference between your normal lumpiness and what may be a change.
Besides a lump or swelling, other changes in your breast might be
- Skin irritation or dimpling
- Nipple pain or retraction (turning inward)
- Redness or scaliness of the nipple or breast skin
- A discharge other than breast milk
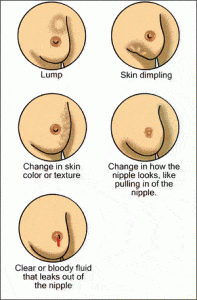
If you see any of these changes, you should see your health care provider right away.
Is there a right way to examine my breasts?
Yes. There are several proper ways to examine your breasts. Ask your health care provider to teach you how to do a breast self-exam to make sure you are doing it correctly and thoroughly. Medline Plus also provides a document that shows the right way to examine your breasts. Click here to visit their website.
Remember that you should discuss any new lump or change with your health care provider.
How often should I do a self-exam?
A breast self-exam is recommended every month a few days after your period ends. During this time, your breasts are less tender or swollen. It is important to do your breast self-exam at the same time every month.
Gynecomastia
Source: American Academy of Family Physicians AAFP
What is gynecomastia?
Gynecomastia is a condition in which firm breast tissue forms in males. The breast tissue is usually less than 1-1/2 inches across and is located directly under the nipple. Gynecomastia may be present on one side or on both sides. This condition may make the breast tender.
Some men and boys have fat on their chests that makes it look like they have breasts. This condition is called pseudogynecomastia (false gynecomastia). It is not the same thing as gynecomastia.
What causes gynecomastia?
Gynecomastia is usually caused by changes in hormones at puberty or as part of aging. Hormones are chemicals produced by the glands of the body, such as the thyroid gland, the testes, and the ovaries. Gynecomastia may be caused by changes in the balance of 2 hormones, estrogen, and testosterone. In rare cases, gynecomastia is caused by prescription drugs, over-the-counter medicines, illegal drugs, tumors or disease.
Are tests needed to find the cause of gynecomastia?
Sometimes tests are needed, and sometimes they’re not. Your doctor will ask you questions about your symptoms, such as how long you’ve had the breast tissue, and whether or not the area is tender. Your doctor will also ask you about the illnesses you have had in the past, the medicines you take, and other matters relating to your health. Then you will have a physical examination.
Whether you need tests depends on your age and what your doctor learns from your history and physical examination. If you are a teenager, you probably will not need more tests, since gynecomastia is common in teenage boys. As many as 65% of 14-year-old boys have gynecomastia. The breast enlargement usually goes away on its own in 2 or 3 years. However, younger boys and adult men with gynecomastia may need to have some tests, because it is possible that some kind of disease is causing the problem.
How is gynecomastia treated?
In most cases, no treatment is needed. Your doctor will probably want to check the size of your breast tissue every few months. In 90% of teenage boys, gynecomastia goes away in less than 3 years.
Sometimes the problem can be solved if you stop taking a medicine that is causing gynecomastia or stop using an illegal drug that is causing the problem.
Occasionally, medicines may be used to treat gynecomastia, especially if tenderness is a problem. The medicine will make the extra breast tissue go away. Rarely, surgery may be necessary to remove the extra breast tissue.
Treatment is necessary if gynecomastia is caused by a disease or a tumor. If it is due to a disease, the disease itself will need to be treated.
Could the breast lump be cancer?
Probably not. Breast cancer is very rare in males. Your doctor will probably be able to tell whether the lump is cancer. Lumps caused by cancer are usually not underneath the nipple, but breast tissue from gynecomastia grows in this area. Breast cancer feels different than the breast tissue of gynecomastia. With cancer, there sometimes is dimpling of the skin or a bloody discharge from the nipple. If there is any question that you have cancer, you will need to have a mammogram and a biopsy.
Mammogram
What is a mammogram?
A mammogram is a test that is done to look for any abnormalities, or problems, with a woman’s breasts. The test uses a special x-ray machine to take pictures of both breasts. The results are recorded on film that your health care provider can examine.
Mammograms look for breast lumps and changes in breast tissue that may develop into problems over time. They can find small lumps or growths that a health care provider or woman can’t feel when doing a physical breast exam. Breast lumps or growths can be benign (not cancer) or malignant (cancer). If a lump is found, a health care provider will order a biopsy, a test where a small amount of tissue is taken from the lump and area around the lump. The tissue is sent to a lab to look for cancer or changes that may mean cancer is likely to develop. Finding breast cancer early means that a woman has a better chance of surviving the disease. There are also more choices for treatment when breast cancer is found early.
Are there different types of mammograms?
There are two reasons mammograms are taken. Screening mammograms are done for women who have no symptoms of breast cancer. Diagnostic mammograms are done when a woman has symptoms of breast cancer or a breast lump. Diagnostic mammograms take longer than screening mammograms because more pictures of the breast are taken.
In January 2000, the FDA approved a new way of doing mammograms, called digital mammography. This technique records x-ray images on a computer, rather than film. It can reduce exposure to radiation, allow the person taking the x-ray to make adjustments without having to take another mammogram, and takes pictures of the entire breast even if the denseness of the breast tissue varies.
Are mammograms safe?
A mammogram is a safe, low-dose x-ray of the breast. A high-quality mammogram, along with clinical breast exam (exam done by a professional health care provider) are the most effective tools for detecting breast cancer early.
How is a mammogram done?
You stand in front of a special x-ray machine. The person who takes the x-rays (always a woman) places your breasts (one at a time) between two plastic plates. The plates press your breast and make it flat. You will feel pressure on your breast for a few seconds. It may cause you some discomfort, feeling like squeezing or pinching. But, the flatter your breasts, the better the picture. Most often, two pictures are taken of each breast – one from the side and one from above. The whole thing takes only a few minutes.
How is a mammogram done in a woman with breast implants?
If you have breast implants, be sure to tell your mammography facility that you have them. You will need an x-ray technician who is trained in x-raying patients with implants. This is important because breast implants can hide some breast tissue, which could make if difficult for the radiologist to see breast cancer when looking at your mammograms. For this reason, to take a mammogram of a breast with an implant, the x-ray technician might gently lift the breast tissue slightly away from the implant.
How often should I get a mammogram?
Women over 40 should get a mammogram every 1 to 2 years. This guideline was just re-issued by the federal government’s U.S. Preventive Services Task Force. And, it is also the position of the Secretary of the U.S. Department of Health and Human Services. Women who have had breast cancer or breast problems, or with a family history of breast cancer may need to start having mammograms at a younger age or more often. Talk to your health care provider about how often you should get a mammogram. Be aware that mammograms don’t take the place of getting breast exams from a health care provider and examining your own breasts.
If you find a lump or see changes in your breast, talk to your health care provider right away no matter what your age. Your health care provider may order a mammogram for you to get a better look at your breast changes.
Where can I get a mammogram?
Be sure to get a mammogram from a facility certified by the Food and Drug Administration (FDA). These places must meet high standards for their x-ray machines and staff. Check out the FDA’s web site on the Internet at: www.accessdata.fda.gov for a list of FDA-certified mammography facilities. Some of these facilities also offer digital mammograms.
Your health care provider, local medical clinic, or local or state health department can tell you where to get no-cost or low-cost mammograms. Also, call the National Cancer Institute’s toll free number 1-800-422-6237 for information on no-cost or low-cost mammograms.
How can I get ready for my mammogram?
First, check with the place you are having the mammogram for any special things you may need to do before you go. Here are some general guidelines to follow:
- Make your mammogram appointment for one week after your period. Your breasts hurt less after your period
- Wear a shirt with shorts, pants, or a skirt. That way you can undress from the waist up and leave your shorts, pants, or skirt on when you get your mammogram
- Don’t wear any deodorant, perfume, lotion, or powder under your arms or on your breasts on the day of your mammogram appointment. These things can make shadows show up on your mammogram
Are there any problems with mammograms?
As with any medical test, mammograms can have limits. These limits include:
- Mammograms are only part of a complete breast exam. If they show abnormalities your health care provider will follow-up with other tests
- False negatives can happen. This means everything may look normal, but cancer is actually present. False negatives don’t happen often. Younger women are more likely to have a false negative mammogram than are older women. This is because the breast tissue is denser, making cancer harder to spot
- False positives can happen. This is when the mammogram results look like cancer is present, even though it is not. False positives are more common in younger women than older women
This FAQ was adapted from mammography fact sheets from the National Cancer Institute.
Endocrine
Thyroid Disorders & Surgery
Surgery to remove the thyroid gland is called Thyroidectomy. Endoscopic Thyroidectomy is a newer, less invasive surgery than the standard “open” Thyroidectomy. The “open” technique involves a large neck incision 6-8 inches or longer, placement of a drain in the incision, and usually a 3-4 day hospital stay.
With the minimally invasive endoscopic approach, the surgery is performed through a smaller incision and most patients are able to go home the same day of surgery.
Benefits of Minimally invasive surgery versus Traditional (Open) Surgery:
- Smaller incision
- Minimal soft tissue trauma
- Less pain
- Faster healing time
- Lower infection rate
- Less scarring
- Less blood loss
- Earlier mobilization
- Usually performed as outpatient day surgery
Endoscopic Thyroidectomy surgery is performed under sterile conditions in a hospital operating room with the patient under general anesthesia. The surgery may be performed by an Otolaryngologist, a head and neck surgeon, or an Endocrine Surgeon.
- You will be placed on your back with your neck hyperextended.
- Your surgeon makes a small incision at the front of the neck.
- The muscles and connective tissue are divided in order to access the thyroid gland and retractors are placed to maintain the operative space.
- Your surgeon inserts the tiny endoscope through the incision.
- Next, the blood supply to the area that is to be removed is clamped off or a special Harmonic scalpel is used which cauterizes as it cuts.
- Both lobes of the Thyroid gland are then removed if a complete Thyroidectomy is being performed. If a partial Thyroidectomy is being performed, then only one lobe of the gland is removed.
- Your surgeon may place a drain to allow fluids to flow out of the area before closing the incision.
- The muscles and tissues are stitched back together and the incision is closed with sutures and covered with a sterile bandage.
Parathyroid Disorders
What are the parathyroids?
The parathyroids are four tiny glands in your neck, two on each side of your thyroid gland. They make parathyroid hormone (PTH) which controls the level of calcium in the blood. Calcium is very important for the normal functioning of muscles, nerves, and bones. It is absorbed through the intestines and stored in the bones. Parathyroid hormone raises blood levels of calcium by increasing intestinal absorption of calcium, and by dissolving calcium from the bone into the bloodstream.
What is hyperparathyroidism?
Some people make too much parathyroid hormone, a condition called hyperparathyroidism. This condition is most common in middle-aged women, but can occur in men or women at any age and can run in families. In 9 of 10 patients with hyperparathyroidism, the cause is a single benign tumor. In one of 10, all four parathyroids are enlarged. Cancer is exceedingly rare.
What are the symptoms of hyperparathyroidism?
The body does not like having blood calcium levels too high, and tells you in a number of ways.
Hyperparathyroidism can cause
- Weak bones, called osteoporosis, which can lead to fractures
- Kidney stones, renal impairment
- High blood pressure
- Abdominal pain
- Increased frequency of urination
- Constipation
- Stomach ulcers and pancreatitis
- Psychiatric problems
- Arrythmias and heart disease
- Difficult to control blood sugar if you are diabetic
- Other symptoms are much more subtle and include
- Weakness and fatigue, loss of energy
- Memory and concentration problems
- Muscle and joint aches and pains
- Abdominal and back pains
- Feeling “older” than you should
- Mood swings or depression
IMPORTANT ***These non-specific, vague symptoms happen with high calcium no matter if it’s only slightly high or very high. High calcium is never normal and should not be “watched.” These vague symptoms improve in 85% of patients after successful parathyroid surgery. Most patients who thought they had no symptoms, in retrospect, realize they did have these symptoms and feel much better within weeks after surgery. They frequently say things like: “I feel 10 years younger,” and “you have given me a new body.” Bone density also improves, reducing the risk of fractures.***
Treatment of hyperparathyroidism
The only effective treatment for hyperparathyroidism is surgery to remove the overactive gland(s). In the hands of an experienced endocrine surgeon, surgery can cure the condition in 98% of cases. There is no effective non-surgical treatment for hyperparathyroidism. Before surgery, you will have a sestamibi scan (a painless scanning test) and a neck ultrasound to see if there is one enlarged gland that can be located.
If the abnormal gland is seen, you can have “parathyroid mini-surgery” through a very small incision, and possibly go home the same day. Even if the gland is not seen, it can still be found at surgery in 98% of cases. The surgery takes about one hour, and the incision is on your neck. You will be completely asleep during the operation and will feel no pain. Recovery is quick, with most patients going home the same day or the next day, and feeling very little discomfort. Most are back at work in a few days!
Frequently Asked Questions
Is there any other treatment besides surgery?
No. Surgery is the only effective treatment of hyperparathyroidism.
What if I don’t have the surgery?
Even if you think you have no symptoms, you will almost certainly feel much better after you are cured. If you don’t have surgery, you will continue to have high blood calcium, and many symptoms listed above. Without surgery, your bones will continue to become weaker, and possibly break. There is evidence of increased risk of high blood pressure, stroke, heart disease, and even shorter life expectancy, from untreated hyperparathyroidism.
How long will I be hospitalized?
Most patients are able to go home the same day (after parathyroid “mini-surgery”) or the following day.
What type of anesthesia will I have?
You will have a general anesthesia. You will be completely asleep during the operation.
When will I know the results of the surgery?
The calcium levels generally return to normal within 12-48 hours of surgery.
Will I have a scar?
Yes. All surgery causes scarring, and how a patient scars are dependent on the individual. However, there are some techniques that surgeons use to minimize scarring. These techniques include careful incision placement and hypoallergenic suture material (to avoid inflammation).For parathyroid “mini-surgery,” the scar is about 1-2 inches. If you need a full neck exploration, it will be bigger. As a general rule, no matter which operation you need, it is unusual to have a very noticeable scar after six months. Scars continue to fade for three years.
Will I have pain after the operation?
All operations involve some discomfort, but most patients are surprised at how little pain they feel after this operation. Although you should be able to eat and drink normally, the main complaint is a sore throat and discomfort with swallowing for 1-2 days. Most patients take over the counter pain meds such as ibuprofen or acetaminophen to keep them comfortable at home. You will have a prescription for something stronger for the first few days in case you need it, but beware prescription pain medicine can make you drowsy and constipated, so do not drive, drink lots of water and eat plenty of fruits and vegetables.
Will I have stitches?
You will have stitches on the inside that dissolve on their own. You will have a waterproof Comfeel dressing so that you can shower or bathe as usual (but do not submerge the incision for 5 days). Leave the dressing in place until your first post-operative visit, where it will be removed.
Will I have any physical restrictions after my surgery?
Your activity level depends on the amount of discomfort you experience. Many patients have resumed golf or tennis within a week after the operation. Most patients return to work in a week, and you are able to drive as soon as your head can be turned comfortably without prescription pain pills (this limitation is for driver safety).
What are the possible complications of parathyroid surgery?
The nerves that control your voice are very closely associated with the parathyroid glands. Temporary voice changes are not uncommon but usually resolve within weeks to months. In 1 in 100 parathyroid operations, the nerves that control the voice are permanently affected. When this occurs, the main difficulties are the projection of the voice and production of high pitched sounds. It is usually described as hoarse, but will not necessarily be considered abnormal by strangers.
Sometimes the surgery will not cure the hyperparathyroidism. In the hands of an experienced endocrine surgeon, failure to cure occurs in fewer than 2 in 100 patients. Sometimes the normal parathyroid glands become “lazy” because the abnormal gland was doing all the work. They may take some time to recover, so some patients require extra calcium tablets on a temporary basis. Rarely, the parathyroids do not recover, and calcium and vitamin D may be needed on a permanent basis. In rare instances, the tumor can recur. Lifelong yearly blood tests are recommended.
There is a small risk of bleeding into the wound. If this happens, it may be necessary to have a second operation to evacuate the blood so it does not interfere with your breathing. Infection is relatively uncommon, and is easy to treat should it occur.
WHAT ARE THE RISKS OF PARATHYROID SURGERY?
As with anything in life, there are risks to surgery. These risks are weighed against the risks of not having surgery. Listed below are some of the possible complications of surgery. Risks include, but are not limited to:
- Permanent voice hoarseness…………………………<1%
- Failure to cure the hyperparathyroidism…………..<2%
- Permanent hypoparathyroidism………………………< ½ % (0% for mini-surgery)
- Infection of Incision……………………………………….Less than 1%
- Haematoma or Bleeding…………………………………Less than 1%
- Seroma (fluid collection)…………………………………1% (temporary)
- Swelling and black/blue………………………………….About 5% (temporary)
- Keloid or overgrown scar…………………………………rare
- Other unforeseen risks
You will require general anesthetic, given by a specialist anesthetist. Risk of a serious complication in a healthy person is very rare. Potential risks include, but are not limited to: - Heart problems (death, heart attack, arrhythmias)
- Lung problems (pneumonia, wheezing)
- Blood clots (stroke, clots in leg veins or lungs)
- Drug reactions (also possible with local anesthetic)
- Chipped teeth
- Other unforeseen risks You will meet the anesthetist before your operation and have the chance to discuss these further.
PREPARATION for SURGERY
- Please shower at home the evening before surgery or in the morning
- Please do not shave the surgical site! It will be done for you if necessary. Shaving yourself may increase the risk of infection
- For morning surgery, Do Not Eat or Drink anything after midnight the night before surgery unless otherwise instructed. This includes coffee, tea, water, and juice! Medication with a small sip of water is OK. For afternoon surgery, a small breakfast BEFORE 7 AM is OK, and nothing after that. Your surgery may be canceled if you do not follow these instructions
- Do Not Drink Alcoholic beverages 24 hours prior to your surgery
- Do Not Smoke for 4 weeks before surgery or your risk of serious complications increases
- Ask us if you are permitted to take your routine medications (such as those for heart, blood pressure, or insulin etc.) before arriving for surgery
- Stop aspirin, warfarin, or any other blood thinner 5-7 days prior to surgery
- Do Not bring valuables such as money, jewelry etc. Do not wear make-up
- Bring toiletries and loose fitting, comfortable clothing to wear upon discharge
- You will be required to remove contact lenses, jewelry, dentures, and wigs
- Arrange for a responsible adult to drive you home after discharge
- Notify us if there is a change in your condition prior to surgery (such as a cold, cough, fever or infection). If severe, your surgery may need to be postponed for your safety
- Stop all herbal medications 4 weeks before surgery unless discussed beforehand. Especially Ginseng, Garlic, and Gingko, or St. John’s Wort, which increase the risk of bleeding
THE DAY of YOUR SURGERY
- If you have not already done so, you will meet your anesthetist
- You may need a blood test or ECG prior to surgery
- After the operation, you will some time in the recovery room before going to the ward After discharge, you are not permitted to:
- Drive a Car nor operate power equipment
- Drink Alcoholic Beverages
Sign important papers
The above are not permitted on the day of surgery, nor while taking any prescription pain medication. Instructions regarding safe resumption of the above activities will be provided by your surgeon.
Post-Operative Instructions for Parathyroid Surgery
Below are general instructions for patients who have had thyroid or parathyroid surgery. Since individual circumstances may vary, it is important that you discuss your individual post-operative care with us.
Monitoring Your Progress
You should feel improvement every day after surgery. If you have any questions regarding your progress, call our office. You should make a follow-up appointment approximately 1-2 weeks after your surgery.
Incision
Your incision is covered with a waterproof protective dressing. You can shower and wash your hair as usual, but do not soak or scrub the dressing. After showering, pat dry. Your dressing will be removed at your first post-operative visit.
If you experience itching once the dressing is off, you may apply lotion to the scar. You might notice bruising around your incision or upper chest and slight swelling behind the scar when you are upright. In addition, the scar may become pink and hard. This hardening will peak at about 3 weeks and may result in some tightness or difficulty swallowing, which will disappear over the next 3 to 4 months. You will also notice some numbness of the skin of your neck. This will gradually improve over time.
Pain
The main complaint following parathyroid surgery is discomfort with swallowing. Some people experience a dull ache, while others feel a sharp pain. This should not keep you from eating anything you want, but the pain can be annoying for a day or two.
You may feel like you have phlegm in your throat. This is usually because there was a tube in your windpipe while you were asleep that caused irritation that you perceive as phlegm. You will notice that if you a cough, very little phlegm will come up. This should clear up in 4 to 5 days.
Voice Changes
Your voice may go through some temporary changes with fluctuations in volume and clarity (hoarseness). Temporary changes are quite common. Generally, it will be better in the mornings and “tire” toward the end of the day. This can last for variable periods of time but should clear in 4-6 months at most. There is a small (1/100) risk of permanent hoarseness.
Hypocalcemia and Bone Health
Your bones have been starved of calcium during the time you have had hyperparathyroidism, and will now have the chance to grow strong again. After successful parathyroid surgery, I recommend you take Caltrate Plus twice a day (available at any chemist) to promote healthy bones. In addition to these supplements, an exercise routine using weights is also recommended.
In about 20% of patients who have parathyroid surgery, the remaining parathyroid glands have become lazy, and do not function properly immediately after surgery. This is usually temporary and causes the blood calcium level to drop below normal (hypocalcemia). Symptoms of hypocalcemia include numbness and tingling in your hands, soles of your feet and around your lips. Some patients experience a “crawling” sensation in the skin, muscle cramps or headaches. These symptoms appear between 24 and 48 hours after surgery. It is rare for them to appear after 72 hours.
Hypocalcemia is treated with extra calcium tablets. You should purchase Calcium with Vitamin D (Caltrate) tablets before surgery so you have them at home. If you feel you need it, take two extra tablets (there is no danger in taking it, even if you do not need it.) The symptoms of tingling/numbness should improve within 30 minutes of taking the tablets. If they do not disappear, you should call my office.
You should repeat the dose whenever the symptoms return. This may mean that you are taking as many as 2 tablets every 3 hours. It is important that you keep us informed. The hypocalcemia should disappear over a few weeks. If it does not, let us know.
CONTACT MY OFFICE for any of the following symptoms:
- Fever >100.5 or chills
- Increasing pain or redness around incision
- Difficulty breathing
- Tingling around the lips or fingertips not relieved by calcium tablets
- Severe muscle cramps
AN IMPORTANT WORD ABOUT THE COSTS OF TREATMENT
Insurance rebates have not kept pace with the cost of running a medical practice. As a consequence, there will be a gap to pay for the surgical fee and for the anesthetist. Your insurance company might also charge you an excess for a hospital admission. We will advise you about expected out-of-pocket costs not covered by insurance. If these costs represent an undue hardship for you, please discuss them with us.
ASK YOUR DOCTOR
We are here to help you. If you have any questions, please ask. It is often helpful to bring a family member with you to a consultation or to write questions down so you won’t forget them.
Adrenal Surgery
Adrenal surgery has been revolutionalized recently with the advent of operative laparoscopy. A laparoscope is like a telescope and through this “minimally invasive” approach an adrenal gland can be removed, thereby minimizing the amount of post-operative pain and the overall recovery period. In some patients with very large tumors of the adrenal gland (>8 cm) or other confounding problems, the laparoscopic approach is not recommended and the standard, larger incision is preferred. However, in most patients requiring an adrenalectomy, the laparoscopic approach is appropriate.
Laparoscopic adrenalectomy is now being performed on a routine basis at our centre. The benefits of the minimally invasive approach are quite clear in regard to postoperative pain and length of hospitalization. Most patients require only a single night hospital stay after the surgery. Patients report a requirement for pain medications that lasts an average of 5-7 days with a “return to normal activities” by 10-15 days. These results represent a significant improvement compared to the standard open adrenalectomy that has been done in the past.

